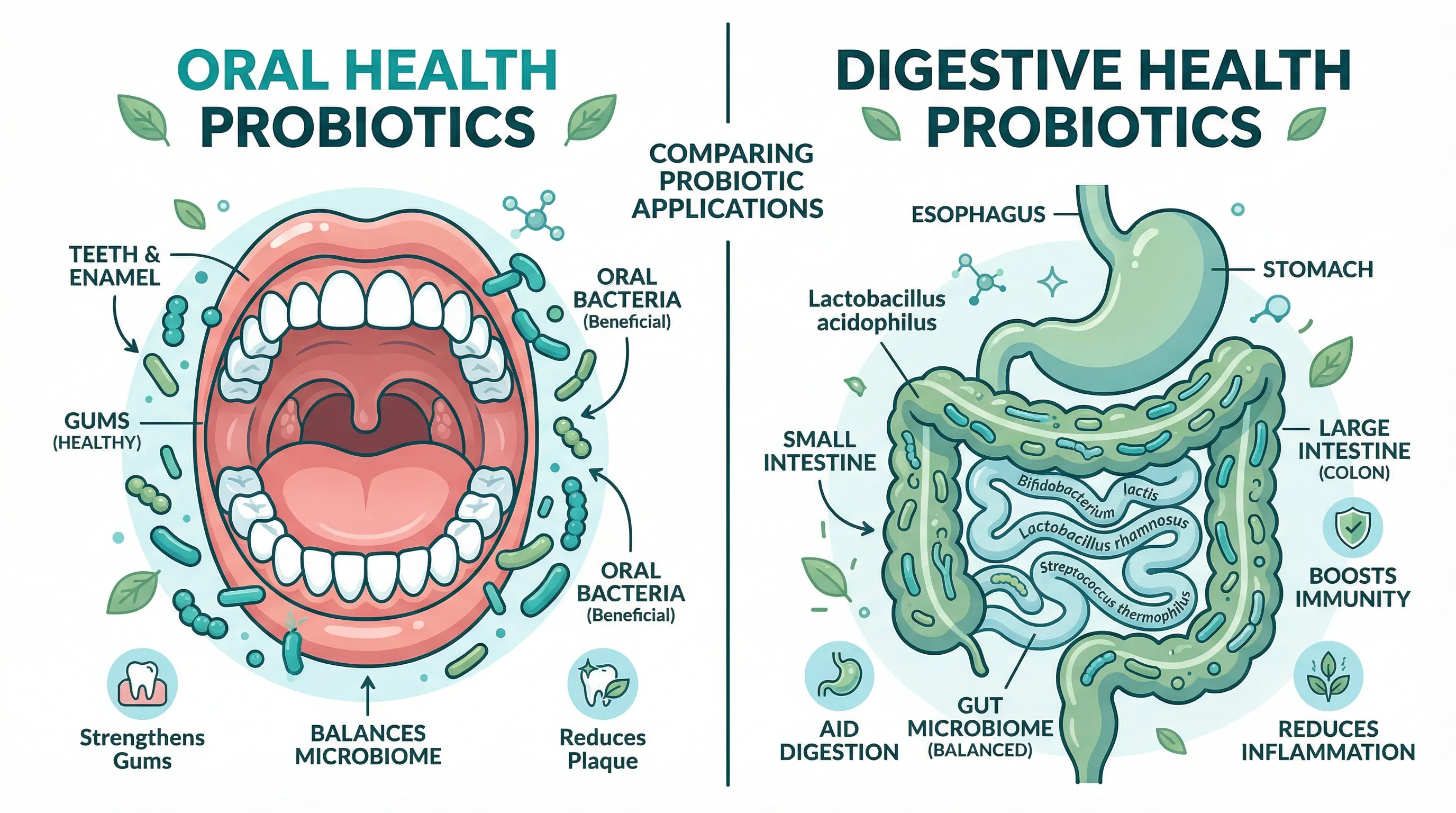
Emerging research suggests that certain probiotic strains — particularly Lactobacillus reuteri and Streptococcus salivarius — may help reduce cavity risk by outcompeting Streptococcus mutans, reducing acid production in dental plaque, and modulating the oral environment. The evidence is promising but not yet definitive. Probiotics should be viewed as a potential complement to proven cavity-prevention strategies (brushing, flossing, fluoride, and regular dental care), not a replacement for them.
Cavities remain the most prevalent chronic disease worldwide. Despite decades of public health efforts — fluoridated water, fluoride toothpaste, dental sealants, and education campaigns — dental caries affects an estimated 2.3 billion people globally, according to the World Health Organization.
The conventional approach to cavity prevention focuses on removing plaque (brushing and flossing), strengthening enamel (fluoride), and reducing sugar intake. These strategies work, but they haven't eliminated the problem. Which raises a question: could manipulating the bacteria responsible for cavities offer an additional line of defense?
That's the premise behind using probiotics for cavity prevention — and the science, while still evolving, is genuinely interesting.
How Cavities Form: A Microbiome Story
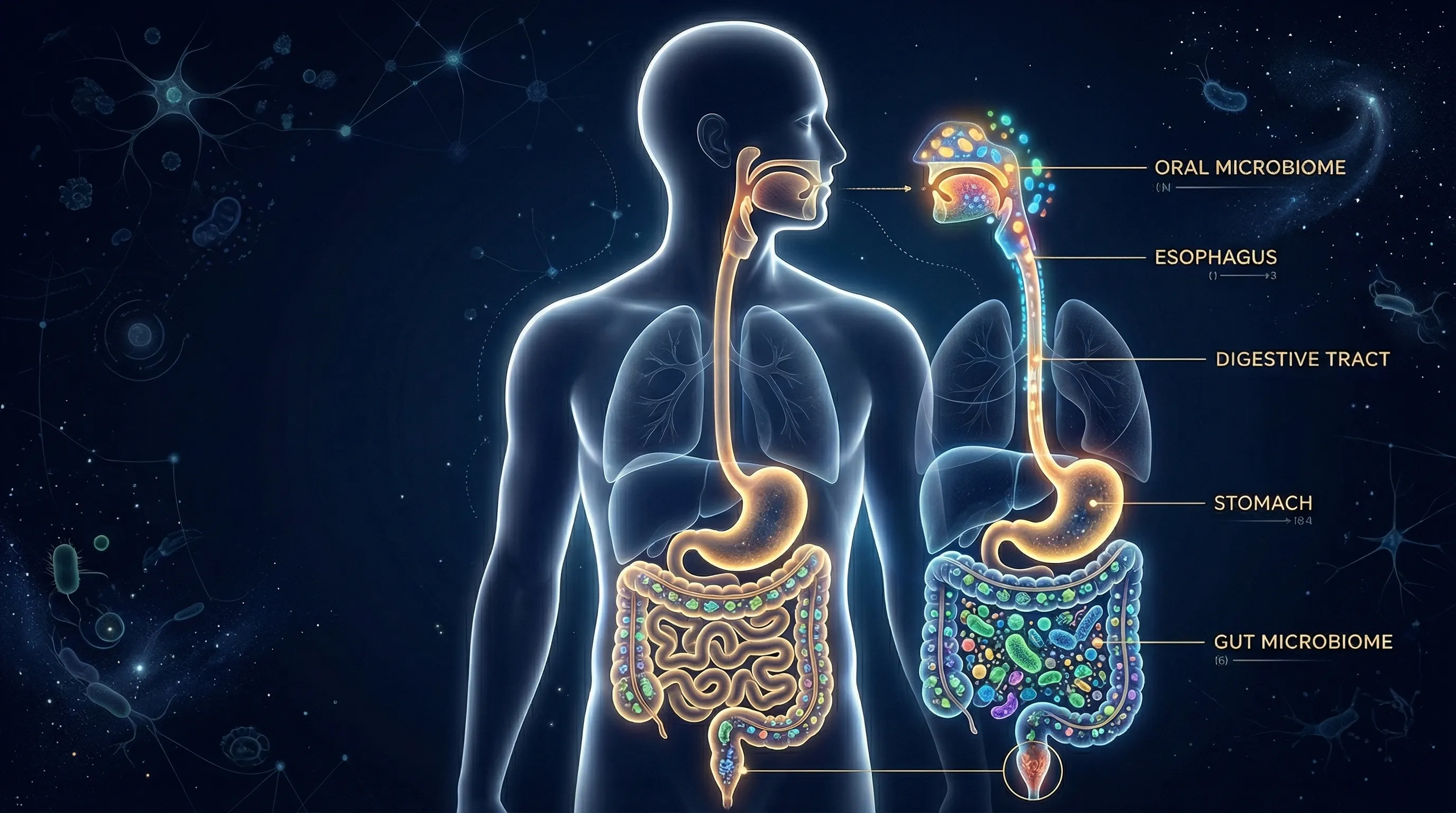
To understand how probiotics might help prevent cavities, you need to understand the microbial process that creates them.
Cavities are not caused by "bacteria" in a generic sense. They're caused by a specific ecological shift within the oral microbiome. Here's the sequence:
- Bacterial colonization: Streptococcus mutans and related species adhere to tooth surfaces within the dental biofilm (plaque)
- Sugar metabolism: These bacteria metabolize dietary sugars (especially sucrose) through fermentation, producing lactic acid as a byproduct
- pH drop: The acid lowers the local pH on the tooth surface below the critical threshold of approximately 5.5
- Demineralization: At this pH, calcium and phosphate ions dissolve out of the enamel matrix
- Net mineral loss: If acid attacks occur more frequently than remineralization (the natural repair process), a cavity forms
The key insight is that cavities are fundamentally an ecological problem. It's not just that S. mutans is present — nearly everyone carries some S. mutans. The problem arises when S. mutans and other acidogenic (acid-producing) species become dominant within the plaque community, creating a persistently acidic environment.
This is where probiotics enter the picture: by shifting the microbial ecology away from acid-producing dominance.
How Probiotics May Prevent Cavities
Researchers have identified several mechanisms by which probiotic bacteria may reduce cavity risk:
1. Competitive Exclusion
The most straightforward mechanism. Probiotic bacteria physically compete with S. mutans for adhesion sites on tooth surfaces and for nutrients in the oral environment. If beneficial bacteria occupy the ecological niches that S. mutans needs, it has fewer opportunities to establish and proliferate.
A study in Applied and Environmental Microbiology (2009) demonstrated that Streptococcus salivarius strain K12 effectively competed with S. mutans for binding sites on saliva-coated hydroxyapatite (a model of the tooth surface), reducing S. mutans attachment by over 95% in laboratory conditions.
2. Bacteriocin Production
Many probiotic strains produce bacteriocins — antimicrobial peptides that specifically inhibit closely related bacteria. S. salivarius K12 produces two bacteriocins, salivaricin A and salivaricin B, which have demonstrated activity against several oral pathogens.
Research published in Probiotics and Antimicrobial Proteins (2013) found that salivaricins were effective against S. mutans strains in vitro, suggesting a targeted antimicrobial mechanism that doesn't cause the broad ecological disruption of antibiotics or antiseptic mouthwash.
3. Acid Production Reduction
Some probiotic strains may help raise plaque pH by consuming lactic acid or by metabolizing sugars through non-acidogenic pathways. Streptococcus sanguinis and Streptococcus gordonii — naturally occurring health-associated oral species — produce hydrogen peroxide rather than lactic acid, creating a less acidic (and less favorable for S. mutans) environment.
A study in Caries Research (2016) found that oral microbial communities with higher proportions of alkali-generating bacteria had lower rates of caries, supporting the idea that shifting microbial metabolism away from acid production is protective.
4. Biofilm Disruption
Some probiotic bacteria produce biosurfactants — molecules that interfere with biofilm formation and stability. By disrupting the structured plaque biofilm, probiotics may reduce the ability of S. mutans to create the enclosed, acidic microenvironments where cavities initiate.
Research in the Journal of Applied Microbiology (2018) found that certain Lactobacillus strains produced biosurfactants capable of reducing S. mutans biofilm formation by 40-60% on polystyrene surfaces.
The Key Strains: What Does the Research Say?
Lactobacillus reuteri
L. reuteri is the most extensively studied probiotic strain for oral health applications. Originally isolated from human breast milk, it produces a broad-spectrum antimicrobial substance called reuterin.
Clinical evidence:
- A randomized controlled trial published in Caries Research (2009) found that school-aged children who consumed L. reuteri-containing milk for 21 months showed significant reductions in S. mutans counts compared to the control group.
- A systematic review in the Journal of Clinical Periodontology (2020) analyzing multiple trials found that L. reuteri supplementation significantly reduced clinical parameters of both caries risk and periodontal disease.
- A study in European Archives of Paediatric Dentistry (2015) reported that L. reuteri lozenges reduced salivary S. mutans counts in children over a 3-week intervention period.
The effect sizes in these studies are moderate but consistent — L. reuteri doesn't eliminate S. mutans, but it appears to reliably reduce its abundance.
Streptococcus salivarius K12 and M18
S. salivarius is one of the most abundant species in the healthy human mouth, making it a logical candidate for probiotic use. The K12 and M18 strains have been specifically selected for their antimicrobial and oral health properties.
Clinical evidence:
- The M18 strain was specifically selected for its anti-caries properties. A clinical trial published in Clinical Oral Investigations (2015) found that children given S. salivarius M18 lozenges for 90 days showed significantly reduced plaque scores and lower S. mutans counts compared to placebo.
- A study in Beneficial Microbes (2016) found that M18 supplementation reduced plaque accumulation in adults, with the effect persisting for the duration of supplementation.
- The K12 strain, better known for its effects against bad breath, also demonstrates competitive exclusion activity against oral pathogens, though its caries-specific evidence is less robust than M18.
Lactobacillus paracasei
L. paracasei has shown the ability to bind to and co-aggregate with S. mutans, potentially interfering with its adhesion to tooth surfaces.
A study in the Journal of Applied Microbiology (2014) found that L. paracasei strain SD1 reduced S. mutans colonization in a clinical trial involving Thai schoolchildren. The effect was attributed to the strain's ability to physically interact with S. mutans and interfere with its attachment to enamel.
What the Evidence Does and Doesn't Show
What the evidence supports
The collective body of research — including multiple randomized controlled trials and systematic reviews — supports several conclusions:
- Specific probiotic strains can reduce S. mutans counts in saliva and plaque
- Probiotic use is associated with reduced plaque accumulation in some populations
- The mechanisms of action (competitive exclusion, bacteriocin production, pH modulation) are biologically plausible and demonstrated in laboratory settings
- Probiotics are safe — no serious adverse events have been reported in oral probiotic trials
What the evidence doesn't yet show
- Long-term cavity prevention: Most clinical trials are short-term (weeks to months) and use surrogate endpoints like S. mutans counts rather than actual cavity formation. Reducing S. mutans is promising, but we don't yet have large, long-term trials proving that probiotic use results in fewer cavities over years.
- Which strain is best: The optimal strain (or combination of strains), dosage, and delivery method for caries prevention hasn't been established.
- Who benefits most: It's likely that probiotics are more effective in some populations (high caries risk, children, elderly) than others, but this hasn't been thoroughly delineated.
- Permanence of effect: Most studies show that probiotic effects diminish after supplementation stops, suggesting that ongoing use is necessary.
A Cochrane review on probiotics for dental caries (Cochrane Database of Systematic Reviews, 2013) concluded that the evidence was "insufficient to determine whether probiotics are effective at reducing caries" — not because the evidence was negative, but because the available trials were too small, too short, and too heterogeneous to draw definitive conclusions.
Since then, additional positive trials have been published, but the overall evidence level remains "promising but not definitive."

ProDentim
Oral Probiotic for Gum & Teeth Health
ProDentim combines L. reuteri — the most studied strain for caries prevention — with L. paracasei and other beneficial bacteria in a dissolving oral tablet designed for direct oral colonization. It represents a practical way to incorporate oral probiotics into your routine.
We may earn a commission if you make a purchase through our links, at no extra cost to you.
Practical Recommendations
Based on the current evidence, here's a balanced approach to using probiotics for cavity prevention:
Probiotics Are a Complement, Not a Replacement
No amount of probiotic supplementation will prevent cavities if you skip brushing, avoid fluoride, and eat sugar all day. Probiotics add a microbiome-management layer on top of proven fundamentals:
- Brush twice daily with fluoride toothpaste
- Floss daily
- Limit sugar frequency (especially between meals)
- See your dentist regularly for professional cleanings and examinations
- Consult your dentist about additional prevention strategies like sealants if you're at high caries risk
Choose Oral-Specific Delivery
For cavity prevention, the probiotic bacteria need to reach and colonize the oral cavity. Swallowing a capsule designed for gut health won't accomplish this. Look for:
- Dissolving lozenges or tablets that release bacteria slowly in the mouth
- Probiotic chewing gums designed for oral delivery
- Probiotic mouthwashes (an emerging category)
The delivery format matters because oral colonization requires sustained contact between the probiotic bacteria and oral surfaces.
Look for Studied Strains
Not all probiotics are created equal. For caries prevention specifically, prioritize products containing:
- Lactobacillus reuteri (the strongest clinical evidence base)
- Streptococcus salivarius M18 (selected specifically for anti-caries properties)
- Lactobacillus paracasei (demonstrated S. mutans co-aggregation)
Generic "probiotic" products without specified strains are unlikely to provide meaningful oral health benefits.
Be Patient and Consistent
The clinical trials showing positive results used supplementation periods of weeks to months. Don't expect overnight results. The process of shifting microbial ecology takes time — you're gradually building up populations of beneficial bacteria and reducing the dominance of acid-producing species.
Consider Your Risk Level
Oral probiotics may be most valuable for people at elevated caries risk:
- Those with a history of frequent cavities despite good hygiene
- Children and adolescents (who have higher caries rates)
- Older adults with reduced saliva flow
- People recovering from antibiotic treatment
- Those with diets that are difficult to optimize (reducing sugar entirely isn't always realistic)
For someone with excellent oral health, good diet, and no history of cavities, the added benefit of probiotics may be minimal.
The Future of Probiotic Cavity Prevention
The field is moving toward more targeted approaches. Research published in Frontiers in Cellular and Infection Microbiology (2020) explored the concept of "replacement therapy" — engineering oral bacteria that occupy the same niche as S. mutans but produce no (or less) acid. While still experimental, this represents a more precise version of the probiotic concept.
Other researchers are investigating probiotic combinations optimized specifically for caries prevention, personalized probiotic recommendations based on individual microbiome profiles, and novel delivery systems (slow-release dental appliances, probiotic toothpastes) designed for sustained oral colonization.
The trajectory of research is encouraging. While we can't yet definitively say "probiotics prevent cavities," we can say that the biological rationale is sound, the clinical signals are positive, and the approach is safe. As larger and longer trials are completed, the picture will become clearer.

ProDentim
Oral Probiotic for Gum & Teeth Health
For those looking to add oral probiotics to their cavity-prevention strategy, ProDentim offers a well-formulated combination of L. reuteri and L. paracasei in an oral dissolving format backed by clinical research.
We may earn a commission if you make a purchase through our links, at no extra cost to you.