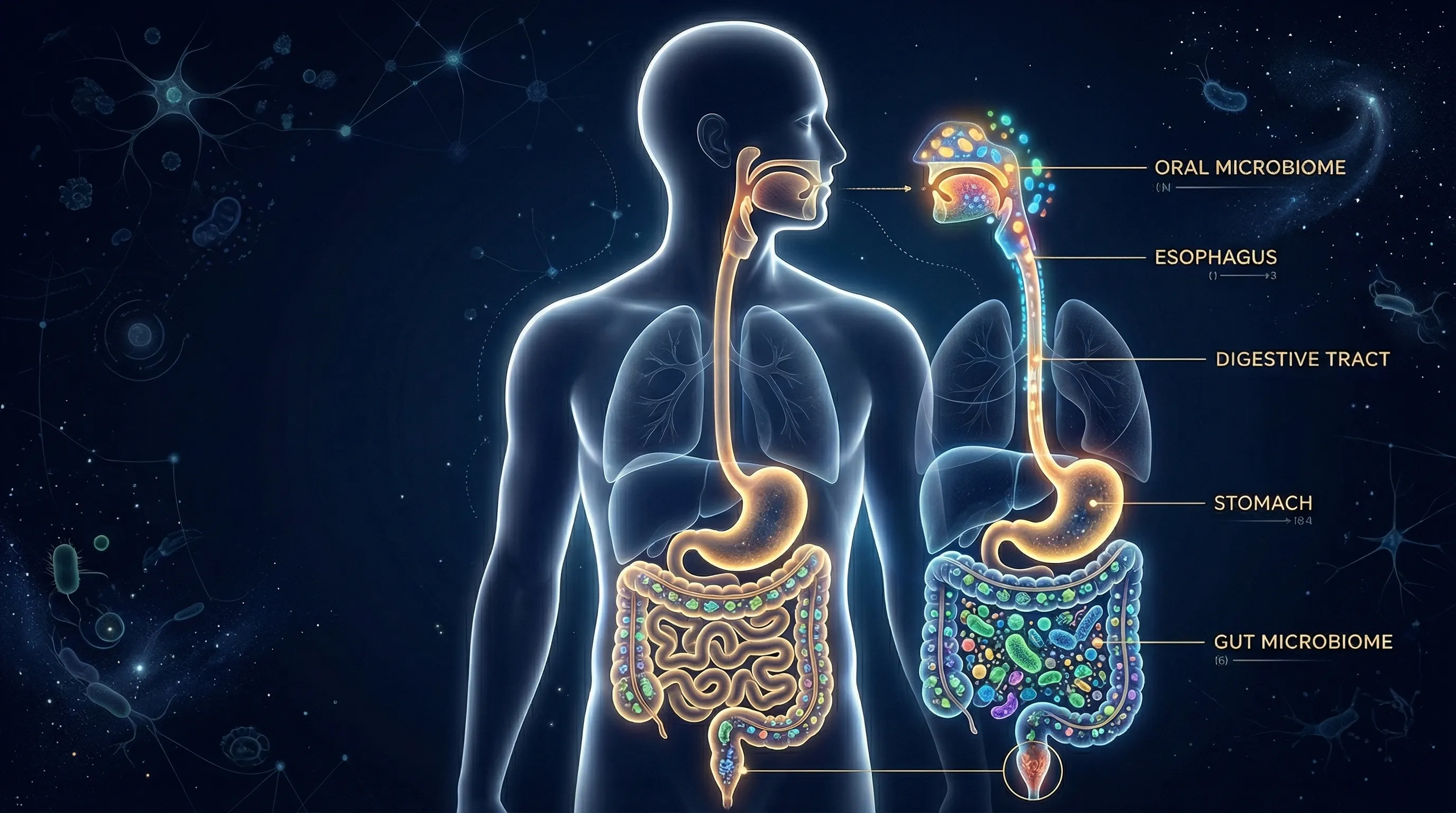
Your mouth and your gut are not separate ecosystems — they are connected through a bidirectional microbial highway known as the oral-gut axis. You swallow roughly 1 trillion oral bacteria every day, and the species that arrive in your intestines can shape digestive health, immune function, and systemic inflammation. Conversely, gut dysbiosis can alter immune responses that manifest in the mouth as gum inflammation, canker sores, and increased susceptibility to periodontal disease. Understanding this two-way relationship is key to protecting both your oral and digestive health.
Most people think of the mouth and the gut as separate systems — one handled by your dentist, the other by your gastroenterologist. But a rapidly growing body of research reveals that these two microbial ecosystems are in constant communication. The bacteria in your mouth don't stay in your mouth. And the condition of your gut directly influences your body's ability to defend your teeth and gums.
This is the oral-gut axis, and it may be one of the most important connections in human health that most people have never heard of.
The Oral-Gut Axis: A Two-Way Microbial Highway
The human gastrointestinal tract begins at the mouth. That simple anatomical fact carries profound microbiological consequences: every time you swallow, you send a bolus of saliva — along with the bacteria living in it — directly into your stomach and intestines.
Research published in Genome Research (2014) used metagenomic sequencing to demonstrate that approximately 45% of the bacterial species found in the gut also reside in the oral cavity. This wasn't a coincidence of similar environments selecting for similar species. Strain-level analysis confirmed that specific oral bacteria were translocating to and colonizing the gut.
A landmark study in eLife (2022) by Schmidt et al. estimated that oral-to-gut bacterial transmission is far more common than previously appreciated — occurring not only in disease states but as a routine daily event. You swallow approximately 1.5 liters of saliva per day, carrying an estimated 1 trillion bacteria from your mouth into your digestive tract.
The communication flows in both directions. Gut immune cells, inflammatory mediators, and even microbial metabolites travel systemically through the bloodstream and influence oral mucosal immunity. When the gut microbiome is disrupted — a state known as dysbiosis — the consequences don't stay confined to the intestines.
When Oral Bacteria Colonize the Gut: P. gingivalis and Disease
Not all oral bacteria that reach the gut cause problems. Many are destroyed by stomach acid or outcompeted by resident gut species. But certain oral pathogens — particularly Porphyromonas gingivalis, the keystone pathogen of periodontal disease — have demonstrated a disturbing ability to survive the journey and alter the gut environment once they arrive.
Inflammatory Bowel Disease (IBD)
A study published in Cell Host & Microbe (2020) by Atarashi et al. demonstrated that oral bacteria, including Klebsiella species originating from the mouth, can colonize the gut and trigger severe intestinal inflammation in genetically susceptible hosts. The researchers found these ectopic oral colonizers in the gut microbiomes of patients with Crohn's disease and ulcerative colitis at significantly higher rates than in healthy controls.
Separately, research published in Journal of Oral Microbiology (2019) showed that P. gingivalis administered orally to mice altered the composition of the gut microbiome within weeks, increasing populations of pro-inflammatory species and reducing beneficial Bacteroides species. The gut didn't just receive P. gingivalis — its entire ecosystem shifted.
Colorectal Cancer
Fusobacterium nucleatum, an oral bacterium commonly associated with periodontal disease, has been found enriched in colorectal tumor tissue. A pivotal study published in Cell Host & Microbe (2013) by Kostic et al. demonstrated that F. nucleatum promoted colorectal carcinogenesis in animal models by creating a pro-inflammatory microenvironment and modulating immune cell infiltration.
Subsequent research in JAMA Oncology (2017) confirmed that high Fusobacterium levels in colorectal tumors were associated with worse patient outcomes, suggesting this oral-to-gut translocation has clinical significance.
Alzheimer's Disease
Perhaps the most striking discovery involves P. gingivalis and the brain. A groundbreaking 2019 study in Science Advances by Dominy et al. detected P. gingivalis and its toxic enzymes — gingipains — in the brain tissue of Alzheimer's disease patients. While the bacteria likely reached the brain via the bloodstream rather than directly from the gut, the oral-gut-systemic pathway is part of the same continuum: oral pathogens that escape the mouth can reach distant organs.
Research published in Journal of Alzheimer's Disease (2020) further suggested that gut dysbiosis driven by oral bacterial translocation may contribute to the neuroinflammatory cascades implicated in Alzheimer's pathology, adding another dimension to the oral-gut-brain axis.

ProDentim
Oral Probiotic for Gum & Teeth Health
Reducing pathogenic oral bacteria like P. gingivalis at the source — in your mouth — may help limit the downstream consequences of bacterial translocation to the gut. ProDentim contains probiotic strains that research suggests may help maintain a balanced oral microbiome.
We may earn a commission if you make a purchase through our links, at no extra cost to you.
How Gut Dysbiosis Affects Your Mouth
The oral-gut axis isn't just about oral bacteria damaging the gut. The reverse pathway — gut problems manifesting in the mouth — is equally significant.
Immune Modulation via GALT
The gut contains roughly 70% of the body's immune tissue, organized in a structure called gut-associated lymphoid tissue (GALT). GALT is where immune cells are educated, activated, and dispatched to mucosal surfaces throughout the body — including the mouth.
When the gut microbiome is healthy, GALT produces balanced immune responses: enough inflammation to fight pathogens, but regulated enough to avoid attacking your own tissues. When gut dysbiosis disrupts this balance, immune cells that migrate to the oral mucosa may be improperly calibrated.
A review in Periodontology 2000 (2021) described how gut-derived Th17 cells — a type of immune cell that drives inflammatory tissue destruction — can migrate to the gums and contribute to periodontal bone loss. The gum disease in these cases isn't caused by local oral bacteria alone; it's amplified by an immune system dysregulated at the gut level.
Systemic Inflammation and Leaky Gut
Gut dysbiosis increases intestinal permeability (often referred to as "leaky gut"), allowing bacterial endotoxins like lipopolysaccharide (LPS) to enter the bloodstream. This triggers low-grade systemic inflammation, which research published in Frontiers in Immunology (2020) has linked to increased severity of periodontal disease, delayed oral wound healing, and higher susceptibility to oral infections.
In other words, a compromised gut may make your mouth more vulnerable to disease — even if your oral hygiene is good.
Oral Manifestations of Gut Disorders
Clinicians have long recognized that certain gut conditions present with oral symptoms. Crohn's disease, for example, can cause cobblestone-appearing oral mucosa, aphthous ulcers, and angular cheilitis. Celiac disease is associated with recurrent canker sores and enamel defects. These are not coincidences — they reflect the shared mucosal immune system connecting the gut and the mouth, as detailed in a review published in the World Journal of Gastroenterology (2019).
The Shared Immune System: Why Both Microbiomes Matter
The mouth and the gut are both mucosal surfaces — lined with mucous membranes that serve as the body's first line of defense against pathogens. They share a common mucosal immune system (CMIS), meaning immune cells activated at one mucosal site can migrate to and influence another.
This has a critical practical implication: you cannot fully address oral health without considering gut health, and vice versa.
Research in Nature Reviews Immunology (2020) described how secretory IgA — the dominant antibody protecting mucosal surfaces — is produced by plasma cells that can originate in the gut and home to the oral mucosa. If gut immune function is compromised, oral IgA production may be impaired, reducing the mouth's first-line defense against pathogenic bacteria.
A study in Mucosal Immunology (2019) further demonstrated that disruption of the gut microbiome with broad-spectrum antibiotics altered immune cell populations in the oral mucosa of mice, increasing susceptibility to oral candidiasis (thrush). The gut and the mouth are immunologically tethered.
Practical Steps: Supporting Both Your Oral and Gut Microbiomes
Understanding the oral-gut axis leads to actionable strategies that benefit both ecosystems simultaneously.
1. Prioritize a Diverse, Fiber-Rich Diet
Dietary fiber feeds beneficial gut bacteria that produce short-chain fatty acids (SCFAs) like butyrate — compounds that strengthen intestinal barrier function and reduce systemic inflammation. A diet rich in vegetables, fruits, legumes, and whole grains supports the gut microbiome, which in turn supports oral mucosal immunity. Research in the British Journal of Nutrition (2018) linked higher fiber intake to lower rates of periodontal disease.
2. Consider Targeted Probiotics
Not all probiotics are interchangeable. Oral probiotics — particularly strains like Lactobacillus reuteri, Lactobacillus paracasei, and Bifidobacterium lactis — have been shown to reduce oral pathogen levels and gum inflammation in clinical trials (Journal of Clinical Periodontology, 2020). By reducing the pathogenic oral bacterial load that translocates to the gut daily, oral probiotics may offer dual benefits.

ProDentim
Oral Probiotic for Gum & Teeth Health
ProDentim delivers targeted probiotic strains directly to the oral cavity, where they may help rebalance the oral microbiome and reduce the volume of pathogenic bacteria you swallow daily — supporting the oral-gut axis from the top down.
We may earn a commission if you make a purchase through our links, at no extra cost to you.
3. Reduce Unnecessary Antimicrobial Use
Broad-spectrum antibiotics and alcohol-based mouthwashes can devastate both the oral and gut microbiomes. A study in mBio (2018) found that a single course of antibiotics altered the gut microbiome for up to 12 months. Similarly, research published in Microbiome (2020) demonstrated that antiseptic mouthwash disrupted the oral microbiome within hours and altered systemic nitric oxide metabolism. Use antimicrobials only when clinically necessary, and discuss alternatives with your healthcare providers.
4. Maintain Consistent Oral Hygiene
Thorough brushing and interdental cleaning reduce the total pathogenic bacterial load in your mouth, which means fewer harmful species translocating to your gut with every swallow. This isn't just about preventing cavities — it's about protecting your entire gastrointestinal tract.
5. Manage Stress and Sleep
Both the oral and gut microbiomes are sensitive to stress hormones and circadian disruption. Research in Psychoneuroendocrinology (2019) linked chronic psychological stress to altered gut microbiome composition and increased periodontal disease severity. Prioritizing sleep and stress management supports both ecosystems.
6. Consult Your Healthcare Providers
If you have chronic digestive issues and persistent oral problems, mention both to your healthcare providers. An integrated approach that considers the oral-gut axis may yield better outcomes than treating each in isolation. Always consult your dentist before making changes to your oral care routine, and your physician before starting any new supplement regimen.
The Bottom Line: Your Mouth Is the Gateway to Your Gut
The oral-gut axis is not a theoretical concept — it is a well-documented biological reality with implications for inflammatory bowel disease, colorectal cancer, cardiovascular health, and potentially even neurodegenerative disease. Every day, the bacteria in your mouth shape the bacterial landscape of your gut, and the immune signals from your gut shape how well your mouth defends itself.
Taking care of your oral microbiome — through good hygiene, thoughtful diet, targeted probiotics, and avoiding unnecessary antimicrobials — is not just about preventing cavities and gum disease. It may be one of the most practical things you can do for your whole-body health.
This article is for educational purposes only and does not constitute medical or dental advice. Always consult your dentist or physician for personalized guidance regarding your oral and digestive health.