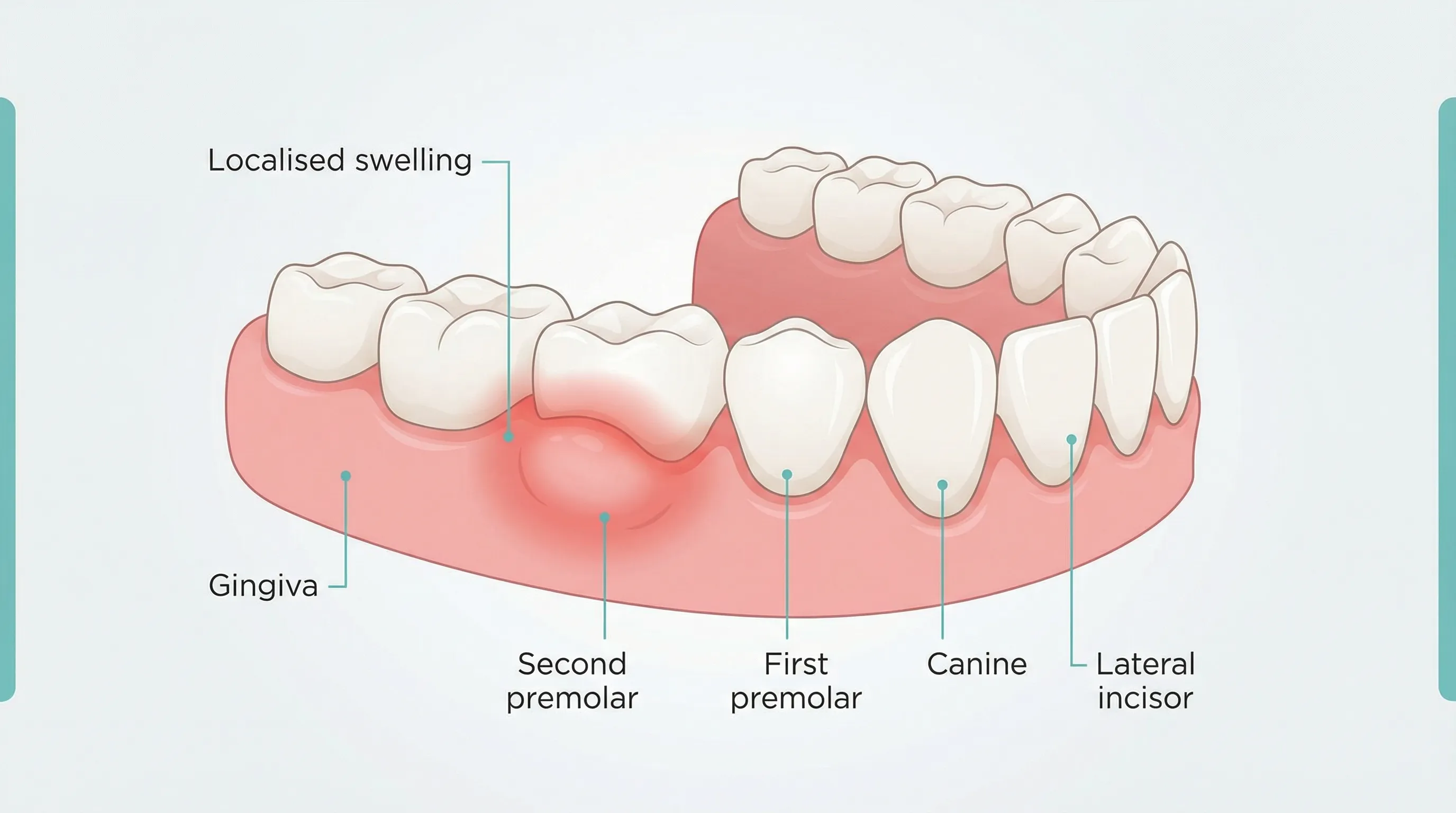
Swollen gums around a single tooth usually point to a localized issue — such as trapped food, a dental abscess, or early-stage periodontal disease — rather than a systemic condition. Most causes are treatable, but an abscess accompanied by fever or facial swelling requires urgent dental care. Consult your dentist if swelling persists beyond two to three days.
When your gums swell up all over, it's usually a sign of generalized gingivitis or a systemic issue. But when the swelling shows up around just one tooth, that tells a very different story. Localized gum swelling is your body's way of flagging a problem in a specific spot — and figuring out what that problem is can save you a lot of pain, money, and worry.
Let's walk through the most common causes, how to tell them apart, what you can do at home for temporary relief, and when you need to pick up the phone and call your dentist.
Why Is Only One Area Swollen?
Generalized gum inflammation tends to stem from plaque buildup across multiple teeth or conditions like hormonal changes and medication side effects. Localized swelling, on the other hand, typically has a pinpointed cause. Something specific is happening at or near that one tooth — whether it's an infection brewing beneath the surface, physical irritation, or tissue damage.
Understanding the distinction matters because the treatment approach can differ significantly depending on the root cause.
Common Causes of Swollen Gums Around One Tooth
1. Food Impaction
This is probably the most common — and most overlooked — cause of localized gum swelling. When a piece of food (popcorn husks are notorious) gets wedged between the tooth and gum tissue or lodged below the gum line, it triggers an inflammatory response.
A 2015 study in the Journal of Periodontology found that chronic food impaction was associated with increased periodontal probing depths and localized attachment loss at affected sites. Even occasional food trapping can cause temporary swelling that feels alarming but resolves once the debris is removed.
Signs it's food impaction:
- Swelling started after eating
- You can feel pressure or a foreign body sensation
- Flossing or an interdental brush brings relief
- The area may be tender but not severely painful
2. Dental Abscess
A dental abscess is a pocket of pus caused by a bacterial infection. There are two main types relevant here:
- Periapical abscess — originates at the tip of the tooth root, usually from untreated decay or a cracked tooth
- Periodontal abscess — forms in the gum tissue next to a tooth root, often related to gum disease
Abscesses are the cause you want to rule out quickly because they can become serious. According to the British Dental Journal (2018), dental abscesses account for a significant proportion of emergency dental visits and, in rare cases, can lead to life-threatening complications such as Ludwig's angina or sepsis if left untreated.
Signs it's an abscess:
- Throbbing, persistent pain that may radiate to the jaw or ear
- A visible bump on the gum (sometimes called a "gum boil") that may drain foul-tasting fluid
- Sensitivity to hot and cold
- Swelling in the face or cheek
- Fever or malaise
3. Localized Periodontitis
Periodontal disease doesn't always affect the entire mouth evenly. Research published in the Journal of Dental Research (2014) has shown that periodontitis can progress in a site-specific pattern, meaning certain teeth may experience deeper pockets and more tissue breakdown than others.
Localized periodontitis around one tooth may result from:
- A tooth that's harder to clean due to position (e.g., wisdom teeth or crowded teeth)
- A defective restoration (filling or crown) with an overhanging margin that traps bacteria
- A history of trauma to that specific area
Signs it's localized periodontitis:
- Swelling that comes and goes over weeks or months
- Bleeding when brushing or flossing around that tooth
- The tooth may feel slightly loose
- Bad taste or odor from the area
- Gum tissue that appears darker red or purplish around that tooth
4. Erupting or Impacted Tooth
If the swelling is around a wisdom tooth (third molar) or in someone younger whose permanent teeth are still coming in, the cause may simply be tooth eruption. The condition of inflamed gum tissue over a partially erupted tooth is called pericoronitis, and it's particularly common around lower wisdom teeth.
A systematic review in Oral Surgery, Oral Medicine, Oral Pathology and Oral Radiology (2016) noted that pericoronitis affects a significant portion of young adults with partially erupted wisdom teeth, with recurrence rates that often make extraction the most practical long-term solution.
Signs it's eruption-related:
- Patient is in their teens or early twenties (for wisdom teeth)
- Swelling is behind the last molar
- Pain when biting down on the tissue flap
- Difficulty opening the mouth fully
- Sometimes accompanied by a low-grade fever
5. Trauma or Injury
A physical blow to the mouth, aggressive brushing over one area, or even biting down on something hard can cause localized gum swelling. Burns from hot food or drinks are another frequent culprit.
Traumatic swelling is usually straightforward to identify because you can typically recall the event that caused it. The tissue may appear bruised (darker than surrounding gums) and is usually tender to touch.
How to Distinguish Between Causes
Here's a practical decision framework:
| Feature | Food Impaction | Abscess | Localized Periodontitis | Pericoronitis | Trauma | |---|---|---|---|---|---| | Onset | Sudden, after eating | Gradual or sudden | Gradual | Gradual | Sudden, after injury | | Pain type | Pressure, mild | Throbbing, severe | Dull ache | Ache, worse biting | Sore, tender | | Fever | No | Possible | No | Possible | No | | Visible bump | No | Often | No | Swollen flap | Possible bruising | | Bleeding | Sometimes | Drainage of pus | On brushing | Sometimes | Yes, if cut |
Home Remedies for Temporary Relief
While home remedies are not a substitute for professional dental care, they can help manage discomfort until you can get to your dentist.
Saltwater Rinse
This is the single most reliable home remedy for oral inflammation. Dissolve half a teaspoon of salt in eight ounces of warm water and swish gently for 30 seconds. Repeat two to three times per day.
A 2017 study in PLOS ONE found that saline rinses reduced bacterial counts and inflammation in oral tissues. The mechanism is straightforward: saltwater creates a hypertonic environment that draws fluid out of swollen tissues (osmosis) and may inhibit bacterial growth.
Cold Compress
Apply a cold pack or ice wrapped in a cloth to the outside of your cheek for 15 minutes on, 15 minutes off. This constricts blood vessels and can reduce both swelling and pain. Cold compresses are most effective in the first 24 to 48 hours after swelling begins.
Gentle Flossing and Irrigation
If you suspect food impaction, carefully floss around the affected tooth. An oral irrigator (water flosser) can also help dislodge trapped debris without traumatizing inflamed tissue. Avoid using toothpicks aggressively — they can push debris deeper or damage gum tissue.
Over-the-Counter Pain Relief
Ibuprofen (if you're not contraindicated) is generally more effective than acetaminophen for dental pain because it addresses both pain and inflammation. Follow the dosing instructions on the package and never exceed the recommended dose.
Hydrogen Peroxide Rinse
A diluted hydrogen peroxide rinse (equal parts 3% hydrogen peroxide and water) may help reduce bacteria around the affected area. Do not swallow the solution, and limit use to a few days to avoid disrupting your oral microbiome balance.

ProDentim
Oral Probiotic for Gum & Teeth Health
Supporting a balanced oral microbiome with targeted probiotic strains like Lactobacillus reuteri and BLIS K-12 — found in ProDentim — may help your gum tissue resist the bacterial imbalances that contribute to localized inflammation.
We may earn a commission if you make a purchase through our links, at no extra cost to you.
When It's a Dental Emergency
You should seek urgent dental care — or visit an emergency room if your dentist is unavailable — if you experience any of the following alongside swollen gums around one tooth:
- Fever above 101 degrees F (38.3 degrees C) — this suggests the infection may be spreading
- Facial swelling — especially if it extends to the eye area, under the jaw, or into the neck
- Difficulty swallowing or breathing — this is rare but constitutes a genuine medical emergency
- Rapidly worsening pain that doesn't respond to over-the-counter medication
- Trismus (inability to fully open your mouth)
The American Dental Association emphasizes that dental infections can become systemic in immunocompromised individuals, people with diabetes, and the elderly. If you fall into any of these categories, err on the side of caution and seek care sooner rather than later.
Professional Treatment Options
The treatment your dentist recommends will depend entirely on the underlying cause:
For Food Impaction
Your dentist will remove the trapped debris and may smooth rough tooth surfaces or adjust restorations to prevent recurrence. If food impaction is chronic, it may indicate a structural problem (open contact between teeth) that needs a new filling or crown.
For Dental Abscess
Treatment almost always involves draining the infection. Depending on the type of abscess, this may mean a root canal (for periapical abscess), incision and drainage, or deep cleaning of the periodontal pocket. Antibiotics may be prescribed if the infection has spread beyond the immediate area. The tooth may need extraction if it's too damaged to save.
For Localized Periodontitis
Scaling and root planing (deep cleaning) of the specific site is the standard first-line treatment. Your dentist may also place a localized antibiotic (such as Arestin) directly into the periodontal pocket. Follow-up visits will monitor pocket depth improvement.
For Pericoronitis
Mild cases may be managed with irrigation, antibiotics, and improved hygiene. However, recurrence is common, and extraction of the partially erupted tooth is frequently the definitive treatment. Your dentist will evaluate whether the wisdom tooth has enough room to fully erupt or if removal is the better long-term option.
For Trauma
Most traumatic gum swelling resolves on its own with conservative care (saltwater rinses, cold compress, soft diet). If a tooth is fractured or loosened by the trauma, your dentist will assess whether it needs stabilization or restoration.
Prevention: Keeping Localized Gum Swelling at Bay
Once you've addressed the immediate cause, prevention is about maintaining strong daily habits:
- Floss daily — particularly around tight contacts where food tends to get trapped
- Use an interdental brush or water flosser for hard-to-reach areas
- Brush with a soft-bristled toothbrush using gentle, circular motions
- Don't skip dental checkups — professional cleanings remove tartar that home care can't
- Address dental work promptly — cracked fillings and poorly fitting crowns create bacterial traps
- Support your oral microbiome — emerging research suggests that a balanced bacterial environment in the mouth may help gums resist localized infections

ProDentim
Oral Probiotic for Gum & Teeth Health
ProDentim delivers probiotic strains that research suggests may help maintain the oral bacterial balance associated with healthier gum tissue and reduced inflammation.
We may earn a commission if you make a purchase through our links, at no extra cost to you.
The Takeaway
Swollen gums around one tooth is almost always a solvable problem. In many cases, it's something as simple as a piece of food stuck below the gum line. But it can also be an early warning sign of an abscess or localized periodontal disease — conditions that are far easier to treat when caught early.
If the swelling doesn't resolve within two to three days of home care, or if it's accompanied by pain, fever, or facial swelling, consult your dentist promptly. Early intervention almost always leads to better outcomes, less invasive treatment, and lower costs.