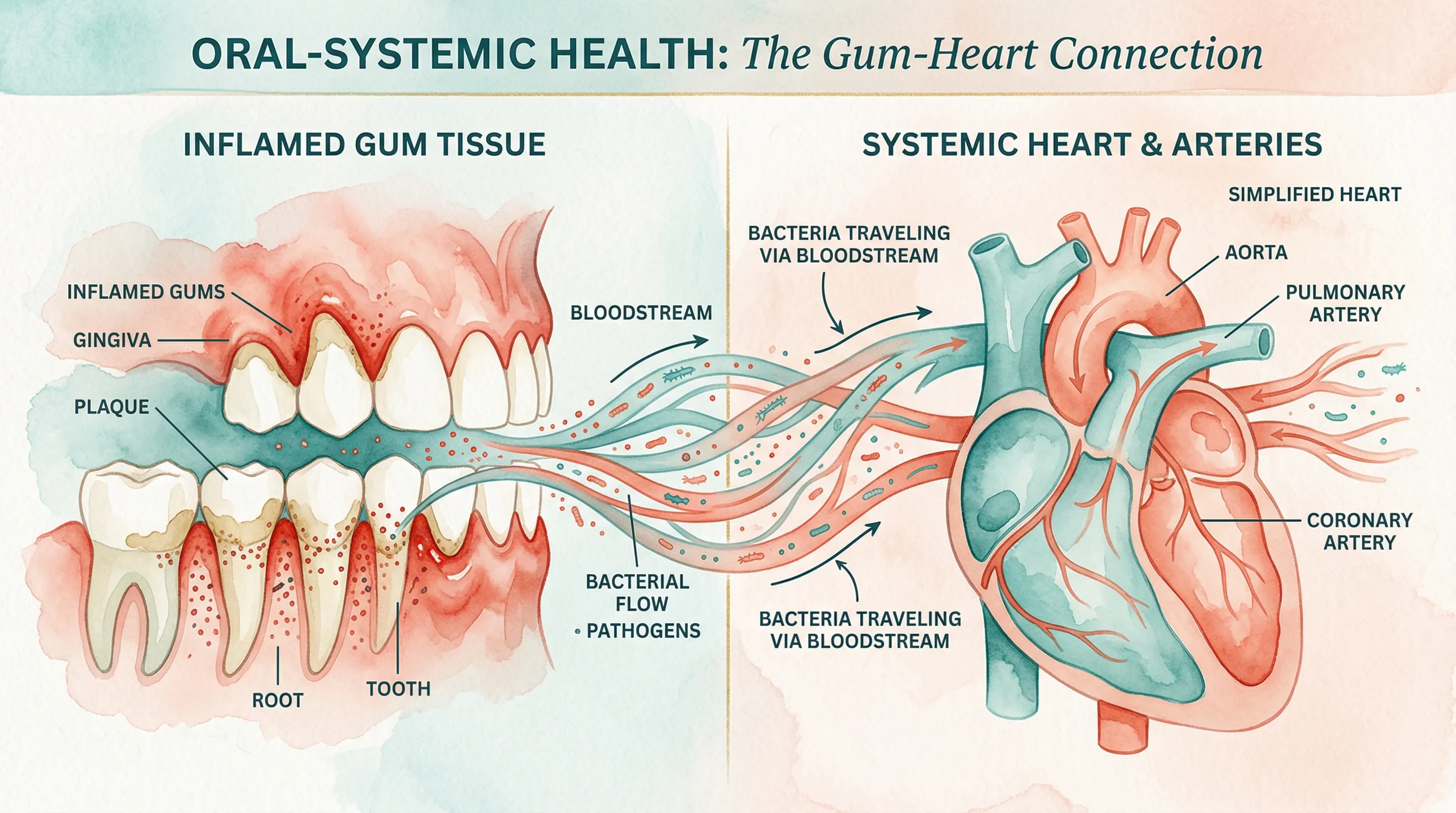
Decades of research have established a significant association between periodontitis and cardiovascular disease. Oral bacteria — particularly Porphyromonas gingivalis — have been found inside atherosclerotic plaques in blood vessels. The shared inflammatory pathways between gum disease and heart disease suggest these are not unrelated conditions. While the relationship may not be simple cause-and-effect, managing periodontal health is increasingly recognized as part of cardiovascular risk reduction.
The idea that your mouth could affect your heart might sound far-fetched. But over the past three decades, a growing body of research has drawn a consistent connection between periodontal disease and cardiovascular disease — one that has captured the attention of cardiologists, periodontists, and public health organizations alike.
Here's what the science actually shows, what it means for you, and what you can do about it.
The Epidemiological Evidence
The association between gum disease and heart disease is not a fringe theory. It's supported by large-scale population studies involving hundreds of thousands of participants.
A landmark meta-analysis published in the Journal of Dental Research (2016) analyzed data from over 7,000 participants and found that individuals with periodontitis had a 20-50% increased risk of developing cardiovascular disease compared to those with healthy gums, even after adjusting for shared risk factors like smoking, diabetes, and age.
An earlier study published in Circulation (2005) — the flagship journal of the American Heart Association — examined data from the ARIC (Atherosclerosis Risk in Communities) study and found that periodontal disease was independently associated with subclinical atherosclerosis, measured by carotid artery thickness.
More recently, a Swedish cohort study published in the European Journal of Preventive Cardiology (2021) followed over 800,000 individuals and found that those who had experienced a heart attack were significantly more likely to have concurrent periodontitis. The relationship held even after adjusting for socioeconomic factors and smoking status.
These are not small studies making speculative claims. This is consistent, large-scale epidemiological evidence.
How Oral Bacteria Enter the Bloodstream
To understand the connection, you need to understand bacteremia — the presence of bacteria in the blood.
Every time you brush inflamed gums, chew food, or even undergo a dental cleaning, bacteria from periodontal pockets can enter the bloodstream through the ulcerated pocket epithelium. In healthy gums, this is a minimal event that the immune system handles easily. But in periodontitis, the total ulcerated surface area inside the pockets can equal the size of the palm of your hand, according to an estimate published in the Journal of Clinical Periodontology (2008).
That's a substantial open wound through which oral bacteria gain repeated access to the circulatory system.
A study in the Journal of Periodontology (2009) detected P. gingivalis in the blood of patients with periodontitis within minutes of tooth brushing. This isn't a one-time event — it happens daily, potentially multiple times per day, for years.
P. gingivalis: The Key Suspect
Among the hundreds of bacterial species in the oral cavity, Porphyromonas gingivalis has emerged as the primary suspect linking gum disease to heart disease.
Research published in Atherosclerosis (2014) detected live P. gingivalis in atherosclerotic plaques removed from patients undergoing carotid endarterectomy (surgery to clear blocked neck arteries). The bacteria weren't just present — they were viable, meaning they had survived in the arterial walls.
A groundbreaking study in the Journal of the American Heart Association (2014) demonstrated that P. gingivalis can:
- Invade endothelial cells (the cells lining blood vessels)
- Promote lipid accumulation in arterial walls
- Stimulate the formation of foam cells — the hallmark of early atherosclerotic plaques
- Increase platelet aggregation, raising the risk of blood clot formation
In animal models, oral infection with P. gingivalis accelerated atherosclerosis in mice, as documented in PLOS ONE (2014). The bacteria didn't just correlate with plaques — they actively contributed to plaque development.
Other periodontal pathogens, including Aggregatibacter actinomycetemcomitans, Tannerella forsythia, and Treponema denticola, have also been detected in atherosclerotic lesions, though P. gingivalis remains the most studied.
The Inflammatory Connection
Beyond the direct bacterial invasion theory, there's a second pathway: systemic inflammation.
Periodontitis is a chronic inflammatory disease. It produces elevated levels of inflammatory markers that enter the bloodstream and contribute to inflammation throughout the body. The same markers are implicated in cardiovascular disease progression:
C-Reactive Protein (CRP): CRP is a systemic marker of inflammation and a recognized independent risk factor for cardiovascular events. A study in the Journal of Periodontology (2010) found that patients with severe periodontitis had CRP levels 2-3 times higher than periodontally healthy individuals. Importantly, research in the New England Journal of Medicine (2005) demonstrated that successful periodontal treatment reduced CRP levels.
Interleukin-6 (IL-6): IL-6 is a pro-inflammatory cytokine elevated in both periodontitis and cardiovascular disease. It stimulates the liver to produce CRP and contributes to endothelial dysfunction — the earliest stage of atherosclerosis. A meta-analysis in Cytokine (2019) confirmed that IL-6 is significantly elevated in periodontitis patients.
Tumor Necrosis Factor-alpha (TNF-alpha): TNF-alpha drives tissue destruction in the gums and also promotes vascular inflammation and insulin resistance. It's a shared mediator linking periodontitis, cardiovascular disease, and type 2 diabetes.
Matrix Metalloproteinases (MMPs): These enzymes break down connective tissue in periodontal pockets and also destabilize the fibrous cap of atherosclerotic plaques, potentially triggering plaque rupture — the immediate cause of most heart attacks.
The critical insight: gum disease and cardiovascular disease may not just share risk factors — they share inflammatory biology.
The AHA's Position
In 2012, the American Heart Association published an official scientific statement in Circulation addressing the relationship between periodontal disease and atherosclerotic cardiovascular disease.
The AHA's conclusions:
- There is a consistent and robust epidemiological association between periodontitis and cardiovascular disease
- The association is independent of known shared risk factors (smoking, diabetes, age, etc.)
- Plausible biological mechanisms exist (bacteremia, systemic inflammation, direct bacterial invasion)
- However, a causal relationship has not been definitively proven — the evidence supports association, not confirmed causation
- There is insufficient evidence that treating periodontitis prevents cardiovascular events (though this reflects the difficulty of conducting such trials, not evidence of no benefit)
The AHA's position is carefully worded: the link is real and biologically plausible, but "gum disease causes heart disease" is a stronger claim than the current evidence supports. What's accurate is that they're connected, and managing one may benefit the other.
What Periodontal Treatment Does to Cardiovascular Markers
If the relationship is driven by shared inflammation, then treating gum disease should reduce cardiovascular risk markers. And that's exactly what research shows.
A systematic review and meta-analysis in the Journal of the American Heart Association (2018) examined 12 intervention studies and found that periodontal treatment (scaling and root planing):
- Reduced CRP levels significantly within 6 months
- Improved endothelial function (measured by flow-mediated dilation)
- Reduced IL-6 and TNF-alpha levels
A study published in the American Journal of Cardiology (2014) found that patients who received periodontal treatment had a 10-15% reduction in carotid intima-media thickness — a direct measure of atherosclerosis progression — compared to untreated controls.
These findings don't prove that gum treatment prevents heart attacks, but they demonstrate that treating periodontal disease measurably improves cardiovascular biomarkers.
What This Means for You
If you have gum disease, you don't need to panic about your heart. But you should take the connection seriously — especially if you have other cardiovascular risk factors like high blood pressure, high cholesterol, diabetes, smoking, or a family history of heart disease.
Steps to protect both your gums and your heart:
1. Get a periodontal evaluation. If you haven't had a full periodontal charting (pocket depth measurements) in the past year, consult your dentist and request one. Knowing your baseline is the first step.
2. Treat existing gum disease. If you have pockets of 4mm+ with bleeding, don't defer treatment. Scaling and root planing is a straightforward procedure that may reduce your systemic inflammatory burden — a benefit beyond just your mouth.
3. Maintain rigorous oral hygiene. Reducing daily bacteremia from inflamed gums starts with twice-daily brushing (Modified Bass technique), daily flossing or interdental brushing, and regular professional cleanings.
4. Support your oral microbiome. The balance of bacteria in your mouth matters. Oral probiotics — particularly Lactobacillus reuteri — have been shown to reduce P. gingivalis levels and decrease gingival inflammation in clinical trials (Journal of Clinical Periodontology, 2020).

ProDentim
Oral Probiotic for Gum & Teeth Health
ProDentim contains L. reuteri and other probiotic strains that research suggests may help reduce pathogenic oral bacteria like P. gingivalis and support a healthier oral microbiome — potentially reducing the bacterial load that enters the bloodstream.
We may earn a commission if you make a purchase through our links, at no extra cost to you.
5. Address shared risk factors. Smoking, uncontrolled diabetes, and poor diet are risk factors for both conditions. Addressing them delivers compounded benefits.
6. Inform your cardiologist about your dental status. If you're under care for cardiovascular disease, let your cardiologist know if you also have periodontitis. Integrated care between dental and medical providers is increasingly considered best practice.
The Bigger Picture: Oral-Systemic Health
The gum-heart connection is the most studied, but it's not the only oral-systemic link. Periodontitis has also been associated with:
- Type 2 diabetes — The relationship is bidirectional. Diabetes worsens gum disease, and gum disease makes blood sugar harder to control (Journal of Clinical Periodontology, 2018).
- Adverse pregnancy outcomes — Periodontitis is associated with preterm birth and low birth weight (British Dental Journal, 2006).
- Rheumatoid arthritis — P. gingivalis produces an enzyme (peptidylarginine deiminase) linked to the autoimmune process in RA (Annals of the Rheumatic Diseases, 2016).
- Alzheimer's disease — P. gingivalis and its toxic enzymes (gingipains) have been found in the brains of Alzheimer's patients (Science Advances, 2019).
These associations reinforce a broader truth: the mouth is not separate from the body. Chronic oral infection has systemic consequences, and gum health may be a more important component of overall health than most people realize.

ProDentim
Oral Probiotic for Gum & Teeth Health
Maintaining a balanced oral microbiome with targeted probiotics like ProDentim may support not only gum health, but the oral-systemic health connection that research continues to uncover.
We may earn a commission if you make a purchase through our links, at no extra cost to you.
The bottom line: you don't need to worry that your bleeding gums are about to cause a heart attack. But the accumulated evidence — from decades of research involving hundreds of thousands of patients — makes a compelling case that taking care of your gums is one meaningful step you can take to support your cardiovascular health. It's not the whole picture, but it's a piece that's too important to ignore.